History of the Hemacytometer
Introduction
The hemacytometer has been an essential tool for hematologists, medical practitioners, and biologists for over a century. Depending on where it is being used, the word has multiple spellings such as hemacytometer, hemocytometer, haemacytometer, or haemocytometer, but for consistency purposes the word “hemacytometer” will be used in this review. The prefix “hema”, “hemo”, “haema”, or “haemo” means blood, while “cytometer” meant a device to measure cells. The device was initially used by medical practitioners to analyze patient blood samples, which was the initial spark that created the field of hematology. The hemacytometer has gone through a series of major development in the 1800s and early 1900s. Detailed descriptions of the development of the hemacytometer were documented in the thesis “The Hemocytometer and Its Impact on Progressive-Era Medicine” by Jack David Davis [1]. Herein, we will provide a synopsis of Davis’ thesis from the beginning of hematology to the instrument modifications that led to the device that is currently used today.
Pioneers in Hematology
Historically, Maxwell M. Wintrobe, Camille Dreyfus, and M. L. Verso were three important physicians and historians who authored numerous groundbreaking publications in the field of hematology. The history of the hemacytometer is closely tied to the rise in the field of hematology, which began in the mid-1700s. The following three pioneers were recognized by Wintrobe as the “Fathers of Hematology”: William Hewson, Gabriel Andral, and George Hayem. Hewson (1739-1774) was a physician and experimental physiologist from England. He was the first to establish that red corpuscles in blood (red blood cells) were individual particles, which engendered the idea that blood particles could be fixed and enumerated. Andral (1797-1876) was a general pathology professor at the Paris Medical School. He was able to measure water, solids, globules, and fibrins in blood by chemical analysis, which allowed him to associate diseases with changes in these elements. Hayem (1841-1933) developed one of the earliest hemacytometer devices for blood counting. He also discovered platelets, made important observations on morphological changes in red blood cells, and documented hematological diseases such as purpura and anemia. Another primary contributor to the field, Paul Ehrlich (1854-1915), was named the “father of chemotherapy”. His work was crucial for the development of colorimetric dyes that allowed physicians to differentiate leukocytes such as granulocytes, lymphocytes, monocytes, eosinophils, and basophils. The hematological research by these pioneers greatly contributed to the development of hemacytometer [1].
Evolution of the Hemacytometer
By the mid-1850s, German scientists had transformed the traditional medical practices from sense and impression (physician’s feeling of patients’ issues) to laboratory medicine by numerical analysis. As a result, the employment of numerous full-time research scientists to teach and experiment initiated the development of the first exact red blood cell counting method by Karl Vierdordt (1818-1884). Vierdordt was a general medical practitioner who became an associate professor at Tübingen. In 1852, he published a paper entitled “Neue Methode der quantitative mikroskopischen Analyse des Blutes” or “New Method of Quantitative Microscopic Analysis of the Blood”, where he described his exact method for red blood cell counting [1]. Vierdordt used a capillary tube with an internal diameter and length of 0.1-0.2 mm and 5-8 mm, respectively. After the blood was drawn into the tube, he was able to measure the internal diameter and length to accurately determine the volume of blood within the tube. Next, the blood sample was expelled from the tube and onto a glass plate coated with egg white, where the sample was allowed to dry. Finally, the glass plate was examined and the cells were counted using a microscope with a square micrometer incorporated into the ocular section. Although this method was tedious and time-consuming, requiring at least three hours for preparation and counting, it was exceedingly accurate.
Vierdordt also published a second article entitled “Zählungen der Blutkörperchen des Menschen” or “Blood Corpuscular Counts in Man”, presenting nine counting results using his own blood, which averaged ~ 5,174,400 cells/mm3 or 5.17 x 109 cells/ml [1]. His work demonstrated the first accurate assessment of red blood cells [1, 2].
Several improvements were made after Karl Vierdordt’s design. Herman Welcker (1822-1897), a student of Vierdordt’s, incorporated ruling on the glass slide in 1854. In 1855, Antonj Cramer (1822-1855) developed a counting chamber by cementing parallel bands on a slide and a thin glass slide on the top to create a volume of 0.011 µl in the chamber. He also incorporated 48 oblong rulings in the microscope to facilitate manual counting that corresponded to a total of 0.172 mm2. This method could determine sample concentration by the known volume in the chamber. In addition, the capillary action allowed for more uniform distribution of the cells [1, 2].
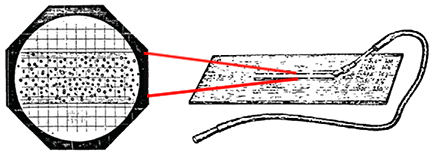
Figure 1. (Right) The capillary tube cell counter designed by Louis Charles Malassez. (Left) The field of view of blood cells in the capillary tube under light microscope with counting grid in the eye piece [1].
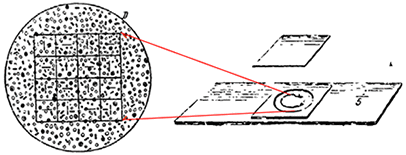
Figure 2. (Right) The counting chamber designed and manufactured by George Hayem. (Left) The field of view of blood cells in circular region under light microscope with a counting grid in the eyepiece [1].
There was no significant advancement in the hemacytometer’s development until 1874, when Louis Charles Malassez (1842-1909) described a new method for counting cells in capillary tubes. While he was an associate director of the Histology Laboratory at the Collège de France, he developed a counting chamber with a flattened capillary tube that was glued to a glass slide with rulings that correlated the length of the capillary tube to volume of samples in the tube (Figure 1). The concentration of cells could then be determined by counting the red blood cells in the tube and multiplying by the dilution factor [1, 2].
Georges Hayem (1841-1933) developed his own hemacytometer chamber in 1875. Onto a glass slide, Hayem cemented a 0.2 mm glass plate with a 1 cm diameter hole, where the thickness could be precisely measured. This method utilized a drop of blood sample directly applied to the center of the glass plate and covered with a cover slip. Because the chamber was not filled by capillary action, sample uniformity was an issue. He then used a microscope incorporated with a square micrometer with a fixed length x width (0.2 mm x 0.2 mm), and was able to determine the cell concentration by multiplying by the measured height of ~0.2 mm (Figure 2). Although Hayem’s device was manufactured and distributed for purchase, it was not well received at that time due to its inconsistency and tedious preparation method [1, 2].
In 1877, William Gowers (1845-1915) made a modified version of Hayem’s hemacytometer that simplified the counting method. He was an assistant professor of clinical medicine at University College in London and published an article entitled “On the Numeration of the Blood-Corpuscles” in 1877 [1]. In the article, Gowers described that only a few blood cell counting instruments had been developed in other countries, and instruments made in Germany or France were inconvenient because the microscope had to be specifically modified and calibrated with the ocular rulings. In order to simplify the state of counting methods, Gowers collaborated with a Mr. Hawksley to develop the first counting chamber with ruling directly on the glass slide, thus eliminating the need to utilize a specialized microscope. The ruling on his chamber was divided into 0.1 mm x 0.1 mm squares, with the height at 0.2 mm, the exact volume could be determined to measure the cell concentration (Figure 3). Later in 1906, he again modified the chamber rulings by changing it to 0.1 mm x 0.2 mm rectangles, but his device was not well received due to the fact that the product did not exist in the trade journal at that time [1, 2].
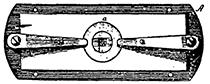
Figure 3. The counting chamber designed and manufactured by William Gowers [1].
The next advancement was developed by Richard Thoma (1847-1923) in 1881. He was an assistant professor at the Pathological Institute at the University of Heidelburg who published a paper with J.F. Lyon, an American physician. His counting chamber was formed by cementing a thin glass plate with an 11 mm diameter hole with a 5 mm diameter glass plate attached at the center, forming a bull’s eye structure. The outer glass plate was 0.1 mm thicker than the inner glass plate, thus forming a natural chamber at a height of 0.1 mm. On the center bottom of the glass slide, a ruling of 1 mm2 area was divided into 16 sets of 25 squares, thus each set of squares was 0.25 mm x 0.25 mm. This chamber was manufactured by the optical company Carl Zeiss and Company of Jena (Figure 4). It was subsequently improved upon by Hawksley, who made the device in one piece, rather than cementing multiple components together. Thoma-Zeiss’ hemacytometer design was designated “the most widely used and most satisfactory instrument for counting the corpuscle” in 1912 by James Campbell Todd, who was a professor of clinical pathology at the University of Colorado School of Medicine [1, 2].
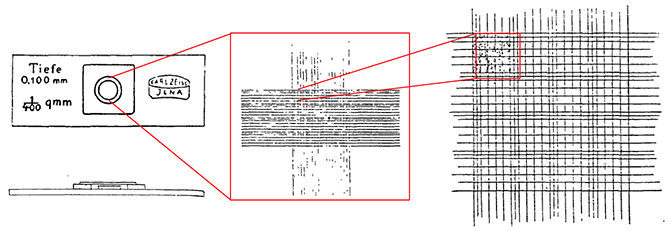
Figure 4. (Left) The counting chamber designed and manufactured by Richard Thoma and Carl Zeiss. (Center) The counting grid etched into the surface of the glass chamber. (Right) A zoomed in image of red blood cells in the grid [1].
At the same time, Louis Charles Malassez developed a second hemacytometer called chamber humide graduée. This device was fabricated by surrounding the sample platform with a ditch at 1 mm deep. The blood sample was applied to the circular surface with rulings and a cover glass was screwed down with four screws to hold it in position. The thickness of the liquid was calculated by the difference between the sample platform and the surrounding surface. Next, water was introduced into the ditch to prevent evaporation of the sample, and then the cells were counted normally [1, 2].
In 1884, Sergei Alferow, a Russian scientist working in Paris, thought it was difficult to obtain accurate blood cell counting due to bad devices and, most importantly, non-uniform distributions of the cells in the counting chamber. Therefore, he developed his own hemacytometer and methodology. His device consisted of isolating the counting platform from the slide by two parallel troughs. The depth was adjusted by four-micrometer screws or glass tubes of known height, where the glass cover slip would be specially designed to fit. The cover slip was secured with two clamps, and the chamber was filled by capillary action (similar to Antonj Cramer’s in 1855) to improve the uniformity of cell distribution in the chamber (Figure 5). Alferow was the first person that took a microphotograph, projected the image onto a glass disc with rulings, and then counted and marked each cell with a pencil. He believed his methodology to be more accurate because the microphotograph was an exact record of the cells present in the counting chamber [1, 2].
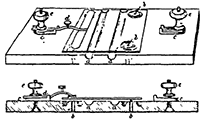
Figure 5. The counting chamber designed and made by Sergei Alferow [1].
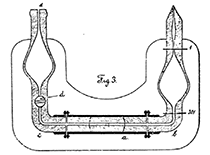
Figure 6. The pipetting and counting apparatus designed and made by W. Brünings [1].
In 1903, W. Brünings of the Pathological Institute of the University of Zürich developed a novel hemacytometer with the ability to mix samples on-chip. The device was connected to a secondary mixing chamber with a pipette and a suction mechanism. After mixing the blood sample in the pipette, it would be transferred directly to a counting field (Figure 6), thus making his hemacytometer one of the first “lab-on-a-chip” devices [1, 2].
The most significant innovation in simplifying counting process and improving accuracy was developed by Karl Bürker (1872-1957). He described the development of his hemacytometer through a series of published articles between 1905 and 1913 [1]. The Bürker hemacytometer was made with a heavy glass slide and three cemented glass platforms on the surface. The three glass platforms were arranged in parallel on the heavy glass, where the middle platform (floor piece at 25 mm x 5 mm) was divided into two parts by a 1.5 mm ditch and with rounded ends on both sides. The two outer glass platforms (21 mm x 7.5 mm) were 0.1 mm higher than the floor piece and separated by 1.5 mm wide channels. When a glass cover slip was clamped over the two outer platforms, a depth of 0.1 mm was formed. On the floor piece, two separate rulings were made, one on each side of the two divisions. The rulings were 1 mm2 that were also divided into 400 small squares (Figure 7). Besides the advantage of the ability to use capillary action to fill the chambers, the hemacytometer had two sides (a double counting chamber) to duplicate counts without the need to re-clean the chamber. With its successive modifications, this device was said to be the best cell-counting chamber by 1921 and had surpassed the Thomas-Zeiss hemacytometer by becoming the most generally used instrument [1, 2].
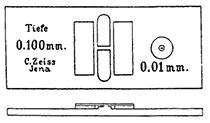
Figure 7. The counting chamber designed and manufactured by Karl Bürker [1].
Improvement in Counting Grids
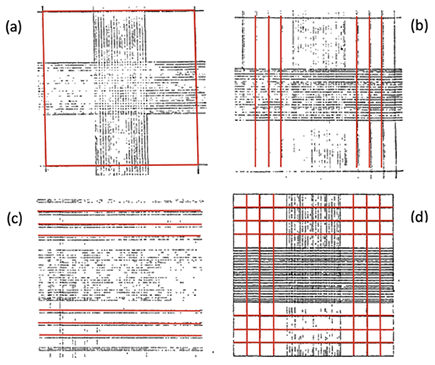
Figure 8. (a) The counting grids designed by J. Zappert by adding external lines to form 9 mm2 of area. (b) Addition of 3 pairs of vertical lines by A. Elzholz. (c) Addition of 3 pairs of horizontal lines by W. Türk. (d) The change of double lines to single lines and combined horizontal and vertical lines by O. Neubauer [1].
The hemacytometer rulings and counting grids have changed many times during its evolution. The counting grid designed by Thoma in 1879 was the foundation for earlier hemacytometers, but as the hematology field advanced, researchers realized that the counting grids were not appropriate for leukocyte measurement because they were mostly designed for counting the smaller red blood cells and platelets.
In 1892, J. Zappert added external lines to form an area of 9 mm2, where nine individual squares of 1 mm2 were formed (Figure 8a). In 1894, A. Elzholz added three pairs of vertical lines in the left and right columns (Figure 8b). In 1902, W. Türk added three more pairs of horizontal lines to Elzholz’s design, thus making the counting grids similar to the ones at present time (Figure 8c). This design replaced the initial Thoma cross grids until 1907, when O. Neubauer changed the lines to single instead of double to simplify the grid layout (Figure 8d), which improved the clarity of the design and became the most used counting grid by 1922 [1].
Summary

Figure 9. (Left) Modern day hemacytometer with double chambers similar to Bürker’s chamber and (Right) Neubauer’s counting grids [3]
For over a century, the hemacytometer has gradually evolved from its simple beginnings, when the field of hematology was in its infancy, to the precisely manufactured instruments used throughout the world today (Figure 9). Although hemacytometer models and techniques still vary, the hemacytometer remains the gold standard for counting cells in both the laboratory as well as the clinic. In the next section, we will discuss the innate sources of hemacytometer error and the basic steps that can be taken to minimize them, thereby increasing the accuracy of cell counting and subsequent in vitro experiments.
References
- Davis, J.D., THE HEMOCYTOMETER AND ITS IMPACT ON PROGRESSIVE-ERA MEDICINE, in Department of History1995, University of Illinois at Urbana-Champaign: Urbana. p. 268.
- Verso, M.L., Some Nineteenth-Century Pioneers of Haematology. Medical History, 1971. 15(1): p. 55-67.
- Rouge, M. Counting Cells with a Hemacytometer. 2002; Available from: http://www.vivo.colostate.edu/hbooks/pathphys/reprod/semeneval/hemacytometer.html.
